Table of Contents
Why Cold Hands Happen
I think it’s safe to assume that anyone reading this has experienced that feeling of freezing cold fingers or toes. For most people, cold hands or feet are the result of being in a really cold environment, holding a block of ice while you fill a cooler for a road trip, or standing in the grocery freezer aisle a little too long. But for others, cold hands are more than a slight inconvenience from time to time. It’s a part of daily life. Medical conditions like anemia, lupus, or scleroderma can cause cold hands. Raynaud’s syndrome (also called “Raynaud’s disease,” “Raynaud’s phenomenon,” or just “Raynaud’s”) is in this category too, and it’s surprisingly common. Experts think that anywhere from five percent to 20 percent of the population might have Raynaud’s. Let’s dig into it a little more to figure out who provides treatment if you think you might have Raynaud’s. A quick side note here: the condition is named after Maurice Raynaud, who first studied the condition back in 1862. It’s pronounced “ray-nose” because, well, it’s French. If it helps, picture yourself wearing a beret and holding a baguette so you feel very French while you say it.
What Is Raynaud’s Disease?
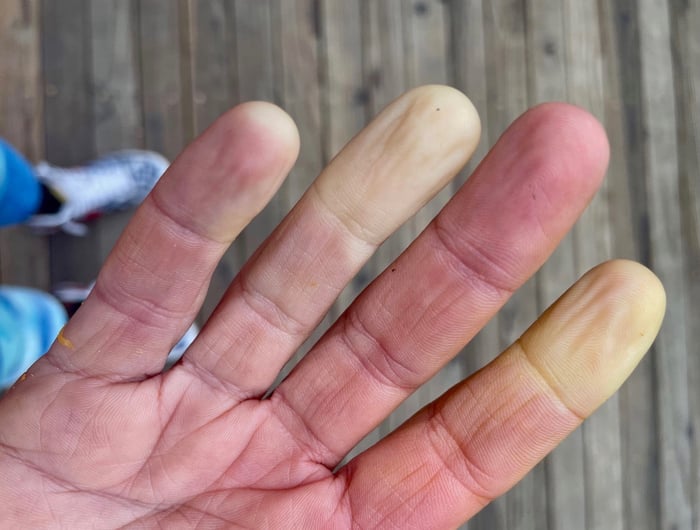
Raynaud’s disease is a condition where the blood vessels contract (meaning they shrink) in response to cold temperatures. Anyone who has been in cold temperatures has probably experienced this already. Your body naturally wants to preserve blood flow to your vital organs, like heart and lungs. When there isn’t enough blood flow to go around, your body will restrict how much blood goes to places like fingers and toes, and redirect it to those vital organs. When you have Raynaud’s your body does the same thing. But it happens more often, and usually in temperatures that are much warmer. You expect to get freezing cold fingers and toes when you stand out in below-freezing temperatures. Someone with Raynaud’s might have that response in any temperature below 70 degrees, for example. The skin may turn white, blue, red, or all three. You might feel numbness and tingling too – that dreaded “pins and needles” feeling when you get cold and warm up again. Raynaud’s can affect other parts of the body besides just fingers and toes, including the nose and ears. Some women also experience a condition called Raynaud’s nipple, with restricted blood flow to your nipples after breastfeeding.
What Kind of Doctor Treats Raynaud’s Disease?
If you have these symptoms more often than you think is normal, or in temperatures where it doesn’t seem like your fingers and toes should be that cold, the next step is to talk to a primary care provider (PCP). The doctor will probably ask you some questions about your symptoms, like when they started, what you feel, and whether you are in pain. Blood tests can also help with diagnosing primary or secondary Raynaud’s. Primary Raynaud’s develops on its own and is more common. Secondary Raynaud’s is the result of another condition. Your doctor might recommend one or more of these tests: Complete blood count (CBC), a test for signs of an infection with a higher-than-normal amount of white blood cells, which could give clues about the cause of your Raynaud’s. Antinuclear antibodies (ANA), a test of how your immune system is working. Someone with an autoimmune disease can have an overactive immune system. Erythrocyte sedimentation rate – a common blood test to check for autoimmune disorders. Nailfold capillaroscopy is a test to check under your fingernails for signs of swelling. This helps doctors determine if you have primary or secondary Raynaud's.
What to Expect After a Raynaud’s Diagnosis
Many people can manage Raynaud’s symptoms with a PCP. But your doctor may refer you to a specialist for additional care. Specialists that commonly work with Raynaud’s patients include: Rheumatologists, who treat joint, muscle, and bone disease, and work with autoimmune disease patients. Cardiologists, who treat issues with blood vessels and circulation. One frustrating thing about Raynaud’s is the lack of treatment options. The advice of most doctors is just to keep your hands and toes warm. But for someone whose fingertips turn white the minute you walk into an air-conditioned office in the summer, that’s not really helpful. You can’t avoid going out in public, and you probably can’t wear ski gloves all day either. There are no medications approved specifically for Raynaud’s treatment right now. But there are some medications your doctor may recommend that can help with symptoms. Surgery is another option. But that’s a big step to take for anyone, and is usually just for people with very severe Raynaud’s disease.
A Helpful Option for Managing Cold Hands
When medications aren’t enough and you really need relief for your cold hands, there is good news. We developed Toasty Touch gloves specifically for people with Raynaud’s (and other conditions, as well as people who just have really cold hands all the time). They are super thin, rechargeable, and stylish. You get unbeatable comfort and ultimate relief from Raynaud’s disease symptoms, no matter how cold it is in your office cubicle or that freezer aisle at the grocery store.
Toasty Touch® Ultra Thin Heated Gloves

$135.00
The heat you need without the bulk. Warm your hands for hours and keep using them with the thinnest heated gloves ever created. “I've finally found something that helps my Raynaud's!” “Life changing!” “Game-changing!” “No more white fingers!” “I've been waiting… read more
FAQs
What are the most common symptoms of Raynaud’s disease?
People often notice cold fingers or toes, color changes in the skin (white, blue, or red), and numbness or tingling when exposed to cooler temperatures.
What kinds of doctors treat Raynaud’s disease?
Rheumatologists and cardiologists are the two specialists most commonly involved in diagnosing and managing Raynaud’s.
| Raynaud’s Symptom | What It Means |
|---|---|
| Cold fingers or toes | Reduced blood flow triggered by cooler temperatures |
| Color changes (white, blue, red) | Blood vessels constricting, then reopening |
| Numbness or tingling | Nerves reacting to decreased circulation |
| Pins and needles when warming up | Blood returning to the affected areas |